Root Canals | Getting to the Bottom of Infections
Posted Dec 2021
By Delta Dental of Arkansas
Tagged mature tooth, crown, anesthetics, infection, pulp, pulpal damage, endodontist, endodontics, root canal
Root Canals | Getting to the Bottom of Infectionsnerve
Think of the worst life has to offer and then some—that’s the reputation of a root canal. As in, “I’d rather have a root canal,” which is what people say to describe something particularly unpleasant.
The saying is way behind the times.
Decades ago, root canals were indeed painful, but nowadays, most people experience little to no pain, thanks to local anesthetics and modern dental advances.
Best of all, a root canal can save a damaged or infected tooth from extraction, therefore preserving your smile by preventing other, more complicated and expensive dental treatments.
Let’s dig deep into root canal specifics.
What is a root canal?
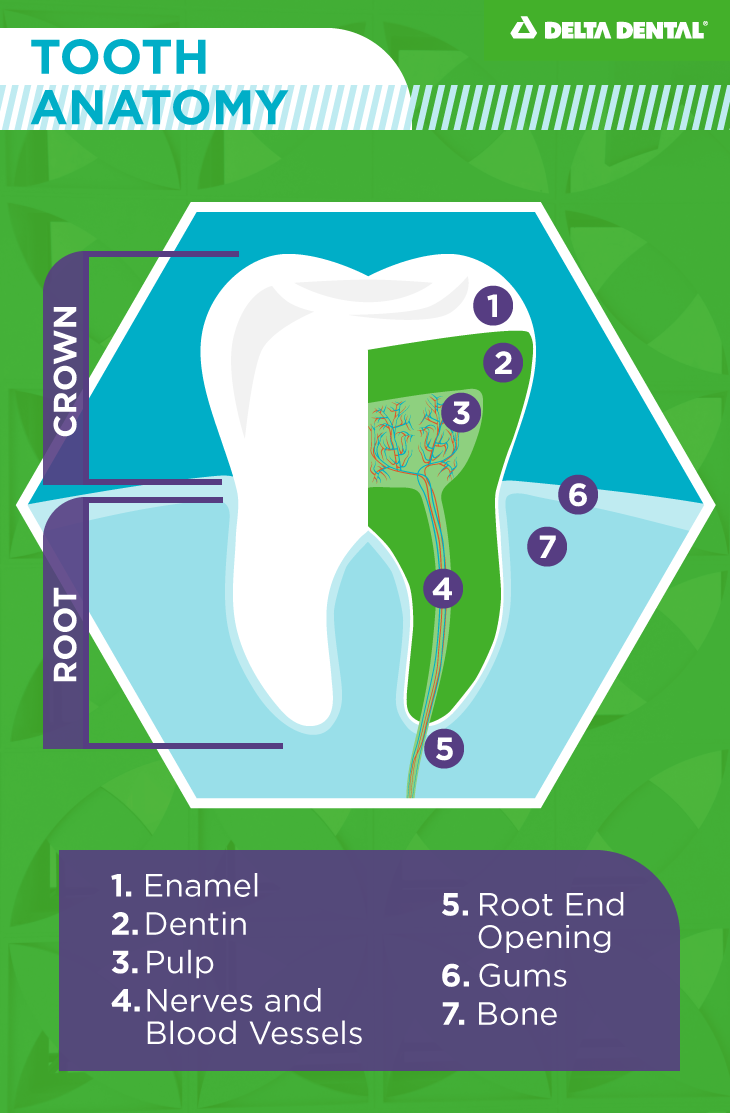
Take a look at the illustration. Beneath the outer layers of tooth enamel and dentin, there is soft tissue called the pulp. It contains blood vessels, nerves and connected tissues, and it goes down all the way to the tip of the roots. If any of these tissues are diseased or the nerve has died, a root canal can be performed to remove the pulpal damage and prevent further decay.
Typically, a root canal will require a trip to an endodontist and a follow-up visit with your general dentist. Some general dentists are trained in endodontics and can do it all.
The procedure consists of 7 major steps:
- A local anesthetic is applied to the diseased tooth.
- A small opening is made in the tooth’s chewing surface or the back side of a front tooth.
- The pulp is removed.
- The chamber is disinfected.
- The canal is filled with biocompatible, elastic material.
- The opening is closed with a temporary filling.
- The temporary filling is removed and replaced with a crown or other restorative treatment during a follow-up visit to your regular dentist.
No pulp, no worries
Although pulp is essential during a tooth’s development and growth, a fully mature tooth can survive without it. It will be nourished by the surrounding tissues.
Causes of tooth decay that might require a root canal
Your dentist may recommend a root canal if your tooth shows signs of infection or nerve damage. The most common causes of pulpal damage include:
- Trauma to the tooth that leads to nerve damage, e.g., a sports injury to the mouth
- A cracked or fractured tooth that allows bacteria to enter the pulp and cause infections and decay
- Severe tooth decay (cavity) that extends down to the nerve or goes through the filling
Signs and symptoms of pulpal damage
How can you tell you might need a root canal? Tell your dentist if you experience any of these signs or symptoms:
- A consistent or recurring toothache
- Tooth pain while chewing
- Tooth sensitivity when eating or drinking hot or cold foods and liquids
- Gum or facial swelling
- Discoloration or graying of the tooth
- Swelling and tenderness of nearby gums
- Drainage from the tooth
Sometimes, no symptoms are present. That’s why it’s important to schedule regular dental check-ups and professional cleanings. Your dentist can identify and address emerging dental issues before they become severe.
How much does a root canal cost?
For insurance purposes, a root canal and the follow-up restorative treatment like a crown are likely to fall into the category of “major services.” Your dental plan may pay 50 to 80 percent of the agreed-upon charges depending on your benefits schedule. A waiting period may apply before you become eligible for insurance benefits for major services.
Check out our cost estimator for approximate charges of dental procedures in your area.
Rooting for you
Since its inception in 1982, Delta Dental of Arkansas has pursued the mission of improving the oral health of all Arkansans through affordable dental insurance for individuals, families and groups. Check out our variety of benefit plans with access to the state’s largest network of dental providers.